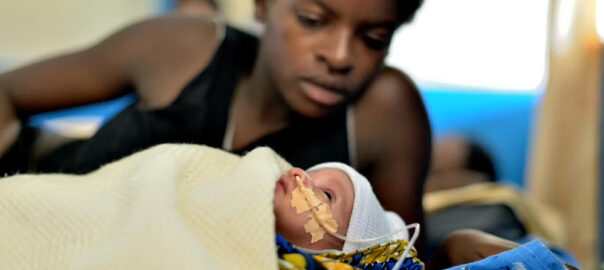
Defense against Infectious Diseases
At least 21 million extra lives were saved due to the accelerated progress resulting from the efforts of the Millennium Development Goals between 2000 and 2015 in child mortality and malaria, maternal mortality, HIV/AIDS and tuberculosis.
Approximately two thirds of those saved were in sub-Saharan Africa, about a fifth in China and India and the remaining numbers in the rest of the developing world.
The importance of Vaccinations
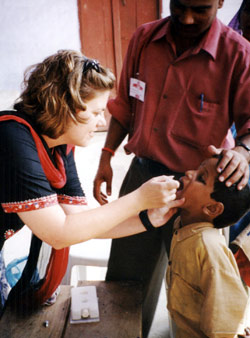
One of the most effective measures of reducing childhood-related death and disability is mass immunization against common infectious diseases. The rationale behind mass vaccination programs worldwide is not only to give the individual protection or a boost to their immune response in the presence of the disease-causing bacterial or viral agents, but to produce community (or herd) immunity. If a large enough proportion of a population has become immune to a disease through infection or vaccination then those not protected, e.g. the chronically ill or the very young and very old, still have a level of protection from getting sick. In the case of measles, for example, 90-95% of the population must be vaccinated to achieve herd immunity because it is very contagious. Polio, which is less contagious, requires 80-85% of the population to be vaccinated.
According to the World Health Organization, “Immunization currently prevents between 2-3 million deaths every year…. It is one of the most successful and cost effective health interventions. An additional 1.5 million deaths can be avoided, however, if global vaccination coverage improved.”
The 2018 Assessment Report of the Global Vaccine Plan reports both good and bad news:
- 116 million infants worldwide received DTP3, the recommended three doses of diptheria-tatanus-pertussis vaccine in 2017 – the most ever.
- The number of under-vaccinated children fell by over 1.8 million between 2010 and 2017.
- Three additional countries achieved maternal and neonatal tetanus elimination – including Haiti – enabling the Region of the Americas to achieve elimination.
- The Western Pacific Region has achieved its lowest ever incidence of measles and its first two countries were verified as having eliminated rubella.
- Immunization activities in the South East Asia Region averted an estimated 622,000 measles deaths in 2017.
- The African Region has seen a 130% increase in government expenditure on immunization since 2010.
- In the Region of the Americas, 33 out of 49 countries have established a platform for immunization of pregnant women.
- The Eastern Mediterranean Region maintained DTP3 immunization coverage at 81%, despite eight out of 22 countries being affected by humanitarian emergencies.
- Two countries in the European Region increased their measles vaccine coverage by more than 10%.
- UNICEF procured over 2.4 billion doses of vaccines for 100 countries in 2017.
The not so good news:
- 9 million children were under-vaccinated in 2017.
- Four out of six regions experienced significant measles outbreaks.
- Several countries and one region – the Region of the Americas – lost measles elimination status.
- Two out of six regions suffered major diphtheria outbreaks.
- A major outbreak of yellow fever in Brazil has been challenging to control.
- 11 countries that had previously achieved 90% DTP3 coverage failed to reach this target in 2017.
- Circulating vaccine-derived poliovirus was detected in three regions.
- Only seven countries reported no vaccine hesitancy in 2017.

The fear of vaccination has many causes. In a WHO/UNICEF study of vaccine hesitancy reported in 2018, respondents gave 1,110 different reasons! Two thirds of the reasons (during years 2014-2016) were based on personal opinions and not on an assessment of the information provided. The top three cited reasons were concerns about 1) risk-benefit or scientific evidence, for example vaccine safety concerns or fear of side effects; 2) lack of knowledge and awareness of vaccination and its importance, for example parents lacking knowledge of immunization benefits; and 3) religion, culture, gender, or socioeconomic issues regarding vaccines, for example certain religious sects or traditional cultural beliefs.
Vaccine hesitancy is a real threat to the continuation of community immunity to the infectious diseases that once ravaged the globe – and still do ravage isolated populations. Providing information and education that address the questions and concerns of parents, at least for those that don’t hold simply anti-vaxxer stances, can make a big difference.
To accomplish large scale vaccination goals, the World Health Organization partners with such organizations as the Center for Disease Control in Atlanta, Georgia (CDC), the United Nations International Children’s Emergency Fund (UNICEF), the World Bank, and private foundations and local governmental public health systems.
The Global Alliance for Vaccines and Immunization (GAVI) initiative is a highly effective partnership combining the technical expertise of the development community with the business know-how of the private sector. Multiple participants support a complex process from identifying the vaccines to be obtained to assuring the long term funding:
- WHO regulates vaccines and supports country introductions, strengthening immunization coverage and data quality.
- UNICEF procures vaccines and supports countries in maintaining their vaccine storage, improving access, and collecting data.
- The Bill and Melinda Gates Foundation provides funding and expertise and supports research on new vaccine development.
- Implementing country governments identify immunization needs, co-finance and implement vaccine programs.
- Civil society organizations help assure that vaccines reach every child.
- Vaccine and equipment manufacturers make available to developing countries affordable, quality vaccines and cold chain equipment (a way for keeping vaccines at correct temperatures).
- Donor country governments make long term funding commitments.
- Other private sector partners contribute resources, expertise and innovation to help achieve success of GAVI.
- Research agencies help generate the evidence base and communicate the value of vaccines.
According to the 2018 GAVI update, the initiative can leverage economy of scale to make vaccine markets larger and more stable and reduce vaccine prices. Higher immunization coverage leads to healthier, more productive populations and greater prosperity. All countries are expected to share in the cost of vaccines, and as their economies improve, they transition away from GAVI support to fund their own vaccine initiatives. Finally, immunization programs put in place a platform for universal health coverage with delivery and surveillance systems that benefit the entire health system, helping to safeguard against disease outbreaks and protect global health security.
GAVI Success Story: Measles Eradication in Cambodia
Cambodia is a good example of what can happen when a country makes a serious commitment to widespread vaccination and is supported by GAVI. Cambodia hasn’t reported a single confirmed case of measles since November of 2011, while its neighbors continue to face outbreaks, illness and death from this vaccine-preventable disease. In 2013, Cambodia became the first low-income (Level 2) country in Asia to protect its children against rubella and congenital rubella syndrome. Cambodia’s success was a three-pronged effort:
Cambodia hasn’t reported a single confirmed case of measles since November of 2011, while its neighbors continue to face outbreaks, illness and death from this vaccine-preventable disease.
1. Measles vaccination: since the early 2000s, Cambodia has placed significant focus and resources on conducting mass measles vaccination campaigns, which led to the dramatic drop in cases. In 2011, a national immunization program began. In May of 2012, a second dose of measles vaccine was provided to all children at 18 months. Two doses of a measles-containing vaccine provides high immunity that lasts a lifetime. In July 2014, CDC immunization experts traveled to Cambodia to evaluate the introduction of the second measles dose into the routine immunization program.
2. Tracking measles and rubella: over the past few years, Cambodian immunization staff integrated their rubella tracking into their measles detection system. This tracking system is sensitive enough to document the disappearance of measles and demonstrate the heavy burden of rubella. Once Cambodia started tracking and reporting cases of rubella and congenital rubella syndrome, the immunization program was able to show that there was a significant burden of disease and successfully applied to the GAVI in 2013 for financial assistance to purchase the 2-in-1 measles-rubella vaccine.

3. Catch-up campaign: with support from GAVI and the Measles & Rubella Initiative, Cambodia conducted a nationwide mass “catch-up” vaccination campaign in November 2013 to protect against measles and rubella in children from 9 months up to 15 years of age. CDC worked with Cambodian health officials to monitor the campaign, which aimed to protect over four million children through vaccination. Health workers traveled to schools all over the country to administer the vaccines to students and set up fixed vaccination sites to reach children under five years of age and children not attending school. CDC’s experts and other national and international counterparts followed the campaign and checked that children were reached, especially those living in remote or underserved communities in rural and urban areas. Advocacy efforts from the Cambodian Government engaged health partners, civil society, community leaders, health center staff and village health volunteers under the umbrella of leadership provided by the Ministry of Health.
GAVI Success Story: Overcoming Vaccine Hesitancy in Nigeria
“Yusuf Ibrahim is a devout Muslim. He is also a convert: not in his religious faith, but in his beliefs about immunisation. Firm-jawed, sitting with his broad shoulders back and his hands placed firmly on his legs, he speaks with passion, recalling a time when he drank in the words of people he considered more learned than himself, accepting them as gospel. ‘Elders told us vaccinations were there to control the population. Everyone believed them – they believed it themselves – so why would I think anything different?’
Western plot
“Rumours that vaccinations are the product of a Western plot to ‘control the Muslim population’ abound in Nigeria, although no one is entirely sure of their origins. Growing up in a tiny farming village an hour away from Minna, Niger State’s capital city, Yusuf was told this as fact. ‘At some point – I don’t recall when – I was told that vaccinations make men impotent. It made sense to us. The elders told us, “Why else would these people who don’t know you give you anything for free? They are doing it for family planning.” And at the time I believed it.’
Near tragedy
“It took a near tragedy to change his heart and mind. Yusuf will never forget the vision of his first-born daughter Saratu, then two years old, when she became dangerously ill. She was coughing and she found it hard to breathe. Then she grew tired, and then limp. His wife begged him for days to be allowed to take her to the doctor and then, with more desperation, to the hospital. As life seemed to drain from her body, her condition raised the spectre of the heart-breaking events that repeatedly befell the small rural community where Yusuf grew up, as young children were snatched from their families.
Pneumococcal pneumonia
“His beloved daughter had pneumonia – an infectious disease that globally claimed the lives of 1.3 million children under the age of five in 2011, of which 129,000 were in Nigeria. ‘I looked at my little girl and I knew what was going to happen,” says Yusuf. ‘When I was a young man I saw plenty of children die. I knew how they looked, and it was my little girl that looked that way now.’
“Yusuf had been told by his village elders to stay away from hospitals and Western medicine altogether. Frantic at the thought of losing his first child, he agreed to allow her to enter a hospital. ‘I don’t know what they did, but they gave my little girl life again,’ says Yusuf.
Preserve life
“He began to talk his beliefs through with the physicians, and gradually they convinced him that they were there simply to preserve life and that had his child been given the right vaccination, she might have been spared this ordeal.
“A decade after his first born faced death and stared it down, Yusuf, now aged 32, is an advocate in his own community: Unguwar Daji, a shanty town without regular power or sanitation services straddling the northern edge of Minna. He makes his way through the maze of streets and orange-dusted back alleys, knocking on the doors of semi-permanent homes with corrugated iron roofs and explaining to families why immunisation is so important.
One of them
“‘If a man’s wife has just had a child, I go and speak to the man and tell him why they need to have a vaccine. And they believe me because I am one of them. We work the same jobs, we are from the same villages, and they see that all of my children have been vaccinated,’ he says.”
Nigeria: States of Change
Gavi.org
GAVI Success Story: Dramatic Child Health Advances in Rwanda
As of 2017 95% of Rwandans were covered by health insurance.
Another vaccination success story is Rwanda, where “close collaboration between the United Nations, international partners and governments, and the Rwandan government produced a dramatic advancement in childhood health. Rwanda’s 97% vaccination coverage rate is one of the highest in Sub-Saharan Africa. Since 1998, Rwanda has decreased its childhood mortality rate from 234 deaths per 1,000 live births to 42 deaths per 1,000 births in 2015, in part due to its increased vaccination rates.” As of 2017 95% of Rwandans were covered by health insurance.
Epidemiology at Work
When a disease outbreak occurs such as cholera, influenza, ebola, Salmonella related diarrhea or food poisoning it is important to quickly identify 1) that it’s occurring, 2) where it’s occurring 3) who was infected first, which can help pinpoint the source and 4) all the contacts that have the symptoms and their contacts so that everyone can be assessed, treated and/or quarantined to help keep the infection from spreading. This is the job of epidemiologists, the investigators of infectious disease outbreaks.
A good example of how training in epidemiology can work occurred during an outbreak of yellow fever in Aweil, Northern Bahr el Ghazal State, in rural South Sudan. As the CDC reported:
“So when surveillance Officer David Deng began investigating, he followed a newly-learned approach that stressed discipline, thoroughness and data. He followed proper investigative procedures and correctly identified the index case (the first person to become ill). With this information, he was able to correctly identify the source of the illness, project its spread and make recommendations to the Ministry of Health. His actions saved many people from getting sick, and may have saved lives. The officer had recently participated in the East Africa Training Project (EATP), and the skills he learned there informed his decisions in this outbreak investigation…
“The techniques and process that the surveillance officer used successfully sprang from CDC’s Global Immunization Division and the Field Epidemiology Training Program. The program was made possible by funding from the Bill and Melinda Gates Foundation. The project has been implemented from 2012-2014 in Ethiopia, Uganda, and South Sudan, which were selected because of their risk for outbreaks of polio and other vaccine preventable diseases (VPDs)…
“The training uses two approaches. First, officers are trained in interactive workshops using presentations, case studies, discussion, field visits to clinics, and contests. Participants learn about topics that are important to immunization, disease detection, and outbreak response. Examples of topics covered include vaccine storage and management, increasing immunization coverage, vaccine safety, waste disposal, case investigation, communications and data collection methods…
“Several Ugandan trainees used their field project to learn why there was low vaccination coverage in their districts. By conducting focus groups with parents, they learned that mothers did not understand the need for repeated immunization visits and did not have transport/fuel to reach vaccination sites. Also, during the rainy season reaching vaccination sites was difficult. The officers shared this information with health center managers and community leaders and opened previously closed outreach sites to increase access to vaccination…
“With support from partners such as the Ministries of Health, WHO, IntraHealth International and the African Field Epidemiology Network, public health officers in Ethiopia, South Sudan and Uganda have increased their core competencies and are better positioned to prevent, detect, and manage VPDs in their countries.”
Malaria, HIV, and Tuberculosis
Vaccines for protection against malaria and HIV are in development, and in the meantime there are other effective interventions that can reduce infection and death. A vaccine called Bacille Calmette-Guérin or BCG, for example, can be effective in protecting against widespread tuberculosis infections in children but it is not as effective in preventing adult TB of the lung. Since the former is rare in the US and using BCG can interfere with TB/tuberculin testing, routine vaccination is not performed here.
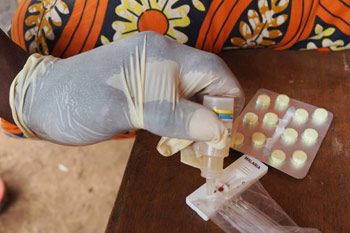
In the case of malaria, the distribution of insecticide treated mosquito bed nets in those areas where the malaria-infected mosquito is present has been effective. Since 2000 over a billion insecticide treated bed nets have been distributed in Africa. Over 6.2 million deaths have been averted from 2000-2015, primarily in children under five and in Sub-Saharan Africa.
The continued improvement of HIV/AIDS treatment has made this infectious disease that attacks the immune system, a survivable chronic disease over the past two decades. According to a 2019 CDC report, “As a key implementing partner of the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR), CDC works side-by-side with ministries of health, civil and faith-based organizations, private sector organizations, and other on-the-ground partners to improve methods for finding, treating, and preventing HIV. The investments made to fight HIV today will save lives and strengthen long-term economic sustainability.”
As of 2018 PEPFAR/CDC has enabled 14.6 million people to receive antiretroviral treatment. Some 11.3 million HIV-positive persons have been screened into care for TB and 813,000 mothers provided antiretroviral treatment to prevent mother-to-child transmission. Efforts towards targeted population messages on safe sex and use of condoms and other barriers during intercourse are also effective and new HIV infections have fallen by 40% between 2000 and 2013.
According to WHO’s Global Health Obervatory (GHO), “Tuberculosis is one of the top 10 causes of death and the leading cause from a single infectious agent (above HIV/AIDS). Millions of people continue to fall sick with TB each year. In 2017, TB caused an estimated 1.3 million deaths (range, 1.2–1.4 million) among HIV-negative people and there were an additional 300,000 deaths from TB (range, 266,000–335,000) among HIV-positive people.
Globally the best estimate is that 10 million people developed TB disease in 2017: 5.8 million men, 3.2 million women and 1.0 million children…two thirds were in eight countries, India, China, Indonesia, the Philippines, Pakistan, Nigeria, Bangladesh and South Africa.” In 2017 there were fewer than 10 new cases per 100,000 in most Level 4 countries.
One of the big challenges is drug resistance. Writes the CDC in a 2017 report:
“Over the years, TB has begun to outwit the drugs used to combat it in the body, leading to drug-resistant forms of the disease. These forms of TB are resistant to our best and most potent drugs, threatening the decades of progress CDC and the global health community has made against the disease…
“Drug-resistant TB exists in two categories: Multidrug-Resistant TB (MDR TB) and Extensively Drug-resistant TB (XDR TB). TB can become resistant to anti-TB drugs when patients are inadequately treated or they are unable to complete their full treatment regimen. Also, drug-resistant TB can be transmitted directly through the air from person-to-person.
“In 2015, there were nearly 500,000 cases of MDR TB, which is resistant to at least two of the first-line anti-TB drugs. This form of TB is now found in every country in the world, with only 1 in 5 people receiving the drugs they need to combat the disease, and of that small fraction, less than half are cured.
“Extensively drug-resistant tuberculosis (XDR TB) is the deadliest and most dangerous form of TB. In most places, less than half of all patients treated are cured, with death rates as high as 80 percent…
“In 2016, CDC helped lead a five-year study in Kwazulu-Natal, South Africa, which provided new evidence that direct transmission, not just inadequate treatment, is driving the spread of XDR-TB. In India, CDC is working with national and local partners to find more cases, improve cure rates, and stop transmission of drug resistant TB in health care facilities, in one of the highest burden countries in the world…
“But more needs to be done. Recent modeling suggests that if left unchecked, eventually TB may no longer be curable and we could see a global resurgence in TB deaths.”
The case of Flora Mugisa in Uganda is but one example of the impact of drug resistance. As is the norm in Uganda’s extended family support system, Flora helped care for her sister when she was diagnosed with a type of tuberculosis that was resistant to several of the antibiotics used to treat it (MDT-TB). Within a year, Flora also fell sick. She lost her appetite, grew thin, and complained of a heavy chest with severe pain.
“I could not sleep at all. I would cough throughout the night. My grandson knew that I would die anytime,” said Flora. She failed to respond to the antibiotic treatment, and she too received a diagnosis of MDR-TB. After 10 months in hospital, Flora recovered enough to be sent back home, where she received daily, directly observed treatment.
After nearly 2 years of treatment, she recovered. She gained weight, had more energy and all of her TB symptoms resolved. “I can now grow my own food. Before, I could not support myself and depended on my neighbors for everything. I now feel strong and happy.”
Tuberculosis prevention, more rapid diagnosis, monitoring of resistant organisms and directly observed therapy (daily monitoring of tuberculosis therapy of infected individuals) has increased cures and reduced resistant tuberculosis which follows from incomplete therapy. Between 2000–2017 an estimated 54 million lives were saved by these efforts.
Global Surveillance
Infectious disease does not respect the sovereignty of either country or individual. With the fluidity of travel across the globe and the presence of vulnerable populations, new and exotic diseases and common organisms like influenza pose a threat of mutating into more virulent organisms.
In 2014 the US experienced its first case of Ebola. The panic associated with the appearance of this highly fatal infection on US soil highlighted the fact that arbitrary borders are not barriers.
Many steps have been taken to establish a global disease surveillance system since early 2000. WHO International Health Regulations (2005) represent an agreement among 196 countries to work for global health security. WHO also created the Global Outbreak Alert and Response Network (GOARN) to provide expertise for epidemiological, laboratory, technical and clinical responses during disease outbreaks. The Public Health Emergency Operations Centre Network (EOC-NET) was established in 2012 to assist and coordinate emergency responses to public health emergencies worldwide. Since its creation the GOARN network has been involved in the investigation of 1471 outbreaks of potential epidemic-prone infectious diseases from SARS to ebola.
In July of 2019, WHO designated the ebola outbreak in the Democratic Republic of the Congo (DRC) a “Public Health Emergency of International Concern” following a confirmed case in Goma, a city of almost two million people on the border with Rwanda. Efforts to contain the DRC outbreak have been hindered by violent conflict in the region, widespread distrust, vaccine shortages, and the lack of global attention which translates to a shortfall in funding and recruitment of additional health workers. WHO’s declaration was based on a number of factors including the year-long duration of the outbreak, its reappearance in spots where it had once been contained, and the expansion of the epidemic hot zone into northeastern Congo near Rwanda and into Uganda.
Fortunately, Uganda has a rich and successful history in global health surveillance achievements. Since 2013, the country has built capacity for surveillance in regional reference hospitals in all of the country’s 118 districts and linked them to National Health Information Systems and the National Health Laboratory System which has been internationally accredited.
To date, smallpox is the only infectious disease to be eradicated globally and that was in 1977 because of the success of worldwide vaccination against the disease.
Makerere University Infectious Disease Institute in Kampala, Uganda has developed a plan to strengthen and coordinate infectious disease surveillance response capacity including prevention and detection in the refugee-hosting districts of Northwestern Uganda. Implementation started in 2017.
From 2016–2017 the Uganda public health emergency operations center responded through a coordinated multi-sectorial effort to multiple outbreaks including: Yellow Fever (2016); Rift Valley Fever (2016); Neisseria Meningitis W135 (2016/2017); Highly Pathogenic Avian Influenza H5N8 (2017); Crimean-Congo Hemorrhagic Fever (2017); multi-drug resistant tuberculosis (2017), Cholera (2017), Anthrax (2017); and Marburg (2017). Time from notification to sample collection to confirmatory diagnosis has been consistently from 24 to 72 hours. Ugandan health worker and Health Ministry officials have been commended by WHO for their sharpened preparedness in responding to the current ebola outbreak centered in neighboring DRC.
To date, smallpox is the only infectious disease to be eradicated globally and that was in 1977 because of the success of worldwide vaccination against the disease.
Antibiotic Resistance and the Future of Global Epidemics
Antimicrobial resistance (AMR) happens when microorganisms (such as bacteria, fungi, viruses, and parasites) change when they are exposed to antimicrobial drugs (such as antibiotics, antifungals, antivirals, antimalarials, and anthelmintics). Microorganisms that develop AMR are sometimes referred to as “superbugs.”
AMR threatens the effective prevention and treatment of an ever-increasing range of infections caused by bacteria, parasites, viruses and fungi. This is an increasingly serious threat to global public health that requires action across all government sectors and society. Without effective antibiotics, the success of major surgery and cancer chemotherapy would be compromised. The cost of health care for patients with resistant infections is higher than care for patients with non-resistant infections due to longer duration of illness, additional tests and use of more expensive drugs. In 2016, 490,000 people developed multi-drug resistant TB globally, and drug resistance is starting to complicate the fight against HIV and malaria, as well.
Antimicrobial resistance occurs naturally over time, usually through genetic changes. However, the misuse and overuse of antimicrobials is accelerating this process. In many places, antibiotics are overused and misused in people and animals, and often given without professional oversight. Examples of misuse include when they are taken by people with viral infections like colds and flu, and when they are given as growth promoters in animals or used to prevent diseases in healthy animals.
In 2016, 490,000 people developed multi-drug resistant TB globally
Antimicrobial resistant-microbes are found in people, animals, food, and the environment (in water, soil and air). They can spread between people and animals, including from food of animal origin, and from person to person. Poor infection control, inadequate sanitary conditions and inappropriate food-handling encourage the spread of antimicrobial resistance.
Antibiotic resistance is present in every country. Patients with infections caused by drug-resistant bacteria are at increased risk of worse clinical outcomes and death, and consume more health-care resources than patients infected with non-resistant strains of the same bacteria.
Daphne Deckers, TV presenter and former top model from the Netherlands who is also a mother of two, suffered from a bladder infection and related health problems for more than a year before doctors found that it was caused by multi antibiotic-resistant bacteria.
“Try to imagine this scenario: you’re sick, very sick. You don’t know what’s going on for a while, then you find yourself in the hospital and the doctors are telling you that out of eight types of antibiotic that usually work to cure a bladder infection caused by E. coli, only one works on yours. Maybe. And if that one antibiotic turns out not to be effective after all, there’s no alternative in place. It’s really frightening. Can you imagine? That, today, you could be diagnosed with a bladder infection that’s become untreatable? That it could actually kill you?”
Daphne’s bladder infection has now been cured, but she worries about whether she’ll get another infection that may not respond to the last type of antibiotic.
As of July 2016, resistance to the first-line treatment for P. falciparum malaria (artemisinin-based combination therapies, also known as ACTs) has been confirmed in five countries of the Greater Mekong subregion – Cambodia, the Lao People’s Democratic Republic, Myanmar, Thailand and Viet Nam. In most places, patients with artemisinin-resistant infections recover fully after treatment, provided they are treated with an ACT containing an effective partner drug. However, along the Cambodia-Thailand border, P. falciparum has become resistant to almost all available antimalarial medicines, making treatment more challenging and requiring close monitoring.
In 2010, an estimated 7% of people starting antiretroviral therapy (ART) in developing countries had drug-resistant HIV. In developed countries, that figure was 10–20%. Some countries have recently reported levels at or above 15% amongst those starting HIV treatment, and up to 40% among people re-starting treatment.
Antiviral drugs are important for treatment of epidemic and pandemic influenza. So far, virtually all influenza A viruses circulating in humans were resistant to one category of antiviral drugs – M2 Inhibitors (amantadine and rimantadine). However, the frequency of resistance to the neuraminidase inhibitor oseltamivir remains low (1–2%).
What’s Being Done
WHO is providing technical assistance to help countries develop their national action plans, and strengthen their health and surveillance systems so that they can prevent and manage antimicrobial resistance. It is collaborating with partners to strengthen the evidence base and develop new responses to this global threat.
WHO is also working closely with the Food and Agriculture Organization of the United Nations (FAO) and the World Organization for Animal Health (OIE) in a “One Health” approach to promote best practices to avoid the emergence and spread of antibiotic resistance, including optimal use of antibiotics in both humans and animals.
A political declaration endorsed by Heads of State at the United Nations General Assembly in New York in September 2016 signaled the world’s commitment to taking a broad, coordinated approach to address the root causes of antimicrobial resistance across multiple sectors, especially human health, animal health and agriculture.
External Stories and Videos

Has our dishonesty prolonged the pandemic and increased the spread of this deadly disease?
UPI
At the height of the COVID-19 pandemic, more than 40% of Americans were untruthful about whether they had the virus or were ignoring safety precautions.


We Can Make COVID-19 the Last Pandemic
Bill Gates, TED
Building a pandemic-free future won’t be easy, but Bill Gates believes that we have the tools and strategies to make it possible -- now we just have to fund them. In this forward-looking talk, he proposes a multi-specialty Global Epidemic Response and Mobilization (GERM) team that would detect potential outbreaks and stop them from becoming pandemics. By investing in disease monitoring, research and development as well as improved health systems, Gates believes we can “create a world where everyone has a chance to live a healthy and productive life -- a life free from the fear of the next COVID-19.”

Has our dishonesty prolonged the pandemic and increased the spread of this deadly disease?
UPI
At the height of the COVID-19 pandemic, more than 40% of Americans were untruthful about whether they had the virus or were ignoring safety precautions.
The Other Reasons Kids Aren’t Getting Vaccinations: Poverty and Health Care Access
Stories about Vaccines, NPR
Religious and ideological opposition to vaccines has fueled the current measles outbreak. But there’s another factor driving low vaccination rates in some communities: poverty.

The Hidden Link Between Farm Antibiotics and Human Illness
Maryn McKenna, Wired
A study years in the making goes further than any other to demonstrate that resistant bacteria can move from animals to humans via the meat they become.

Toilets for the World
National Geographic
Nearly a billion people still defecate outdoors. The problem isn’t just a lack of toilets—it’s a lack of toilets that people want to use, The result” millions of deaths and disease-stunted lives.
Ebola Updates
World Health Organization
WHO provides weekly updates on the DRC ebola outbreak, declared a global health crisis in July 2019.

Q&A: Rwanda prepares for the risk of Ebola
Rebecca Root, Devex
In what it calls the “pre-epidemic phase,” the Rwanda Red Cross has been conducting simulations with its staff and volunteers as well as taking part in national simulations conducted by the Ministry of Health in the event that the outbreak spills into Rwanda.

